Preparing for a Pandemic
Clinical operations ramped up quickly to care for COVID-19 patients
By Robert C. Jones, Jr.
They had been watching the crisis unfold for weeks, reading and viewing the news reports of patients who were gravely ill from a mysterious pneumonia-like illness and were packing the wards of hospitals in Wuhan, China.
They watched as the virus marched across Europe and reached the United States by plane and by cruise ship, straining the resources of health care facilities that were fighting not only to save lives, but also to replenish badly needed medical supplies.
Eventually, the coronavirus that causes COVID-19 would make its way to South Florida, and when it did, vowed pulmonologist and critical care specialist Tanira Ferreira, M.D., the University of Miami Health System and its 560-bed UHealth Tower hospital would be ready.
“We started planning and preparation back in January, and as we saw the situation evolve, we mobilized our efforts,” said the assistant professor of medicine and chief medical officer of UHealth Tower, referring to the team of which she is part that has marshaled resources and manpower so that UHealth’s clinical operations can deal effectively with the first truly global threat of this century.
To care for the influx of COVID-19 patients the hospital would see, a task force of physicians, nurses and administrators changed the way health care is being administered at UHealth Tower, creating special units and teams dedicated to the care of those patients, ramping up screening protocols, and instituting a host of hospital-wide measures to make sure the virus doesn’t spread.
A Reinvention
UHealth Tower’s north and south penthouse floors were converted to COVID-19 units, with patients quartered in negative-pressure isolation rooms that allow air to flow in but not out — a ventilation technique that prevents the escape of aerosolized viral particles.
Teams of physicians and nurses, culled from the hospital’s existing intensive care unit, were created with the purpose of caring solely for those patients. They’ve been equipped with the resources they need to do their jobs effectively. UHealth’s coronavirus task force, acutely aware of the rising worldwide mortality rates of COVID-19 patients, created ICU environments with telemetry monitors in each of the negative pressure rooms.
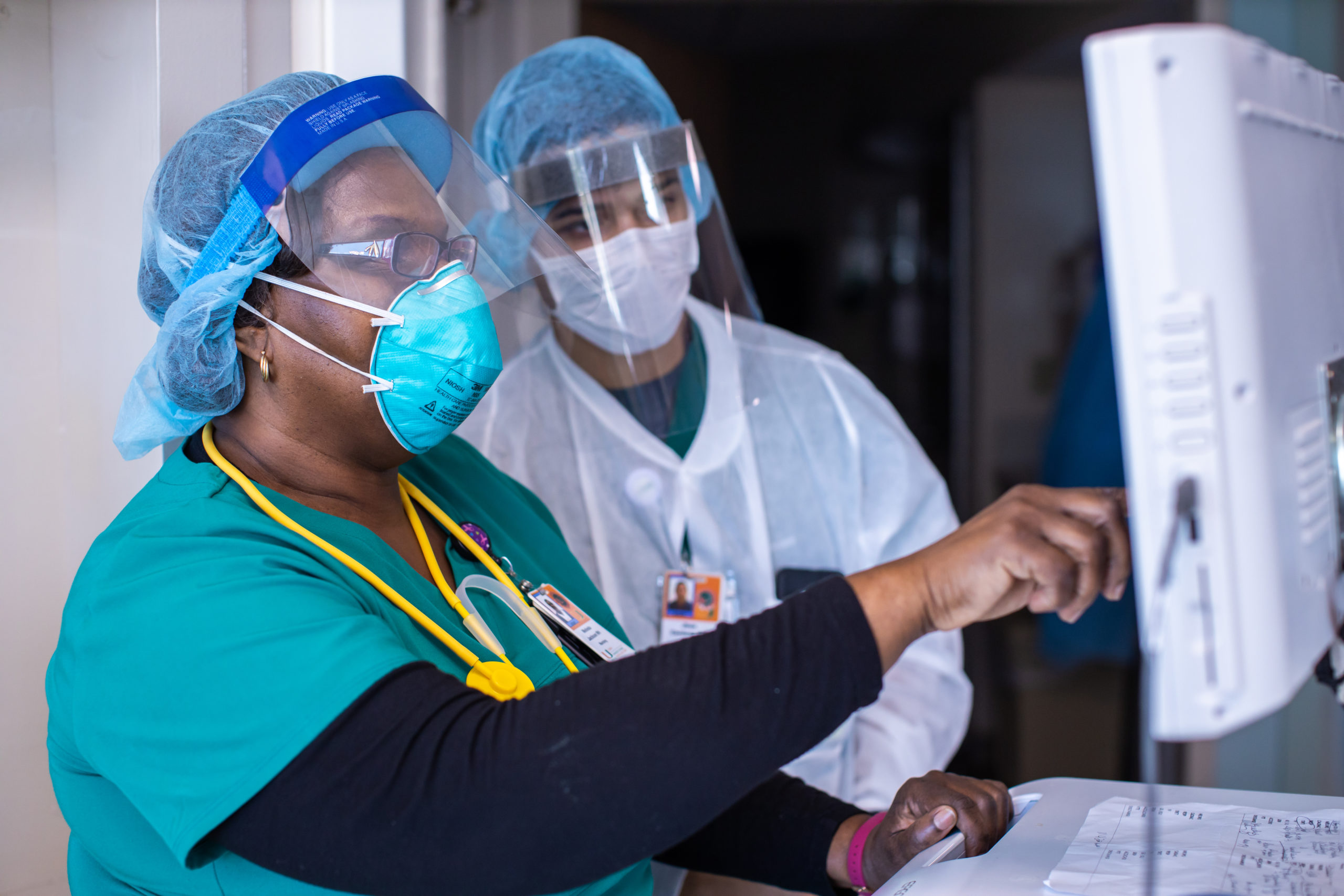
Physicians and nurses were caring for 43 coronavirus patients on the penthouse level in mid-April. In the event that unit reached capacity, additional beds were standing ready on the south tower’s tenth, eleventh and twelfth floors, where negative-pressure environments had also also been created, bringing to 149 the total number of beds dedicated to COVID-19 patients.
As of then, the issue of having enough space — a pressing concern for many hospitals around the country that were facing shortages as the coronavirus outbreak worsened — had been addressed by UHealth leadership.
“But that doesn’t mean we’re not constantly looking for more rooms and adjusting our plans for a surge in cases, which could be anywhere from 400 to 600 patients. We’re just not sure yet,” said Kymberlee Manni, Ph.D., the CEO of UHealth Tower.
Drs. Manni and Ferreira, and Chief Operating Officer Dipen Parekh, M.D., are three of the key players in UHealth’s clinical response to the coronavirus outbreak and the expected surge in patients the health system is expecting.
“We need to remain focused for the long road ahead,” Parekh, a renowned urologic oncologist, said in a recent video message to UHealth employees. “Getting through this will mean each of us stepping in and doing our part.”
The response has been all-encompassing, “a total reinvention of ourselves,” Dr. Ferreira said.

An Emergency Department at the Ready
That reinvention is prevalent throughout UHealth Tower, beginning on the ground with its Emergency Department, where tents have been erected outside to screen patients. There, medical staff ask patients a battery of questions that range from whether they are experiencing fever, cough or respiratory symptoms to their recent travel history to countries hit hard by the virus. Anyone who presents a positive response is placed in an isolated area.
Certain rooms within the ED have been designated as isolated areas for high-risk patients.
“We consider every patient who comes in to possibly have coronavirus,” said David Lang, D.O., medical director of UHealth Tower’s Emergency Department. “Some are a little bit easier to detect; they come in with fever, cough, shortness of breath. But we also see patients who come in with something totally unrelated and who need to be admitted for other illnesses, but who can test positive for the virus.
“So our process has changed,” Dr. Lang continued. “The entire department now wears masks, and we have masks on the patients. When we go in to see patients, we put on protective gear. If it’s high risk, it may be a little bit more gear, and if it’s lower risk, we may not fully suit up. But our approach is to consider every patient a suspect.”
New triage practices have been implemented to see the “walking well” — patients who may have a fever but are generally healthy — outside in the special tented area, where medical staff can diagnose and discharge them quickly without having to bring them inside.
“Plans are reviewed every day as the volume and complexity of patients changes and as we learn more about how to treat these patients and what their needs are,” Dr. Lang said.
He and his staff of physicians and nurses have watched news reports in sadness and empathy as their colleagues at hospitals in New York, now the epicenter of the pandemic, battle to keep patients alive with limited capacity and supplies.
“All the physicians in my department have friends or relatives working in New York, doing emergency medicine. So we get first-hand accounts from them,” Dr. Lang said. “So far, for us, it’s been nothing like that. But the patients we do see remain sick. We’re still a tertiary medical center and see things that other departments and other hospitals can’t manage. We get our fair share of complicated medical and surgical patients. We still provide services for oncology. So those patients who are already immunocompromised from chemotherapy can’t be mixed with COVID-19 patients in the same area.”
Dr. Lang has practiced emergency medicine in Miami for 25 years, experiencing the anthrax and Ebola scares and seasonal influenza. The coronavirus pandemic, he said, is unlike anything he has ever seen. “We’re seeing it in college students, in nursing home patients — it has affected everyone.”
For Richard Zaidner, M.D., associate medical director and one of the attending physicians for UHealth Tower’s Emergency Department, the biggest change in the way he has practiced clinical medicine as of late has been the manner in which he prepares to see patients.
“We know the virus is pretty virulent and spreads rather quickly, and obviously our concern is not to spread it in our hospital community or take anything home,” Dr. Zaidner said. “So we’re diligent about wearing our PPE [personal protective equipment] and being very cautious.”
That means changing into clean and sanitized scrubs that are waiting for them at the hospital when they arrive for their shifts and then donning masks, face shields and gloves.
“We gown up for patients who could potentially have it,” Dr. Zaidner said, “and if we’re doing invasive procedures like intubation, that’s when we go into full PPE, a closed system where there’s really no exposure at all.
“We see every patient and want to make sure they’re in good hands,” Dr. Zaidner continued. “Yes, we’re putting ourselves at risk, but it’s worth it; we want to make every patient better.”
“We see every patient and want to make sure they’re in good hands. Yes, we’re putting ourselves at risk, but it’s worth it; we want to make every patient better.”
— Richard Zaidner, M.D.
He and the other ED staff leave their scrubs behind when their shifts end, changing back into civilian clothing. And to minimize the risk of contaminating his residence and spouse, Dr. Zaidner, like many of the other doctors and nurses, undresses outside when he returns home, tossing the garments he wore underneath his scrubs into the washing machine on the hot-water cycle and jumping into the shower.
UHealth, he said, was “ahead of the game” before the hospital even admitted its first COVID-19 patient.
“We met pretty early on before this even started, making the decision to cohort patients who have any respiratory symptoms away from every other patient in the ED so we’re not cross-contaminating,” he explained. “We have the tents outside, and then we have isolation areas inside. So it’s almost like we have two separate emergency departments.”
A total of 36 fully recovered patients have been discharged. But the hospital hasn’t hit its peak, warned Dr. Ferreira.
“It’s like tracking a hurricane,” she said. “Everyone wants to know where it will strike. In this case, we’re asking, ‘When will the number of cases hit its peak?’ The models seem to align over the last week of April or first week in May.”
Dr. Ferreira starts her day early, answering the 30 or so emails received overnight as she managed to get what little sleep she could. Once at the hospital, she huddles virtually with leadership, then ensures that whatever action items have been decided are executed.
She had already conferenced in on two meetings and taken several calls before the clock hit 10 a.m. one recent Wednesday. And as Ferreira has done every day since UHealth Tower began caring for COVID-19 patients, she rounded, going to each floor to ask health care providers “what they need, what’s working, and what is it that’s not working.”
Life Inside UHealth’s COVID-19 Unit
It is mid-afternoon on a Wednesday, and Joseph Falise, nurse manager for the cardiovascular ICU and the neuroscience intensive care unit, is well into his shift at the COVID-19 unit on the penthouse floor, overseeing staffing, patient care, and supplies, and collaborating with physicians to ensure the unit is running smoothly.
He takes a moment to reflect on what medical personnel in New York are facing, noting that he and others at UHealth have participated in conference calls with and received feedback from ICU staff who are working in what is now the center of the pandemic.
“The patient acuity here isn’t any different than what’s in New York,” Falise said. “What is different is we don’t have as many patients. But the therapies we’re trying are all very similar to what’s happening in New York. Putting [patients] on a ventilator is one thing. Everything else is the hard part, turning them on their stomachs — what we call proning — to increase their oxygenation. All the things that we do only once in a while in the ICU we’re doing to almost every patient now.”
Bedside dialysis, he said, is being done continuously, and even some clinical trials have been initiated, with one UHealth physician using a new therapy that has the potential to delay the need for a ventilator for COVID-19 patients. In that trial, pulmonologist Roger Alvarez, D.O., M.P.H., began treating a COVID-19 patient in late March, using a nitric oxide system called INOpulse that had been recently approved by the FDA for treating coronavirus patients.
“The cardiopulmonary benefit demonstrated by INOpulse in various indications provides the potential to prevent deterioration in patients with COVID-19, allowing ventilators to be preserved for the most critically ill,” explained Dr. Alvarez, referring to the system developed by Warren, N.J.-based Bellerophon Therapeutics, Inc.
Extensive Protocols
All told, more than 30 protocols dealing with how to care for COVID-19 patients have implemented, with everything from medication and oxygenation procedures to cardiac care being considered. Even special rules dealing with how to transport such patients within the hospital were created.
“That’s a huge endeavor in itself,” Dr. Manni said. “It takes an entire team — security to clear the hallways and then housekeeping to clean the pathways and inside the elevators going and coming.”
And then there is testing.
“You’ve got to make sure you’re getting the patients tested and getting the results back quickly,” Dr. Manni explained. “When we saw that we weren’t getting timely reports from the Florida Department of Health, some our rapid action teams got together to secure additional equipment and test kids to help turn results around faster.”
UHealth has gotten a “fairly good jump” on obtaining medications and supplies as well, she said.
Stocking Up
Keith Murphy, vice president for UHealth Supply Chain Services, and his team started ramping up PPE supplies before the first case of COVID-19 was even confirmed in the U.S., on one occasion placing an order for 100,000 masks from one of the health system’s suppliers.
“We had been watching the situation in China and knew what was coming,” he said. “Gowns, shoe covers, masks, goggles — all the PPE you see medical professionals wearing. It’s really all of that and above,” Murphy said of the storehouse of personal protective equipment his team acquired for clinicians. “Everyone was put on allocation from normal suppliers, so we were tasked with finding alternate sources, and we did.”
In all, Murphy’s team worked with 19 medical supply companies—nine of which are traditional UHealth suppliers — to purchase the equipment that was needed. And since their efforts started in earnest earlier this year, they have been able to acquire 1.2 million N95 masks, the gold standard for the protection of healthcare workers caring for patients; 1.5 million surgical masks; 5,000 reusable face shields; 250,000 disposable face shields; 100,000 isolation suits; and 200,000 isolation gowns.
His team also has rented 28 ventilators, 17 bilevel positive airway pressure units, 18 anesthesia machines, 40 portable suction units, and 25 patient stretchers to supplement UHealth’s existing supply of that equipment.
He ordered adequate reserves of hand sanitizer and disinfectant wipes, aggregating the bulk of all supplies for UHealth Tower.
“The teamwork has been amazing, everyone pulling together. Should a surge in COVID-19 cases come, we’ll be prepared.”
— Keith Murphy, vice president for UHealth Supply Chain Services

From left, Keith Murphy, Jose Corredor, Luis Vargas, Raquel Avellar and Nate Yuen.
Photograph by Sonya Revell.
Monetary gifts and in-kind donations have also helped Murphy’s team to maintain adequate supplies for medical staff. One philanthropist donated 270 gallons of hand sanitizer, which is being sent to a local hand-sanitizer manufacturer who will pour it into one- and two-ounce bottles that will be branded with the UHealth logo and given to employees, according to Nate Yuen, executive director of value analysis for UHealth Supply Chain Services.
Supply Chain Services worked with a team of 13 buyers and managers, generating more than $20 million in coronavirus-related purchases.
In partnership with Academic Purchasing, Supply Chain Services worked with a team of 13 buyers and managers, generating more than $20 million in coronavirus-related purchases.
With supply and demand often creating desperate competition among buyers worldwide, driving up the cost of many items to several times their normal price, Team U had to mix high-tech sourcing with old-fashioned negotiating. Still, UHealth got what it needed — and in time.
“The teamwork has been amazing, everyone pulling together,” Murphy said. “Should a surge in COVID-19 cases come, we’ll be prepared.”
A number of different projects, addressing everything from resource utilization to research and clinical trials that could speed therapies to patients, will undoubtedly have an impact on clinical care for COVID-19 patients, said Bhavarth Shukla, M.D., assistant professor of clinical medicine and director of Infection Control, which is overseeing those initiatives.
Among some of the projects: novel ways of disinfecting N95 masks and face shields; developing a UV disinfection system based on protocols created at the University of Nebraska National Ebola Treatment and Education Center; and a hydrogen peroxide vaporization disinfection model.
“We’ve already piloted the UV model and started using it,” Dr. Shukla said.
Waging a War
U.S. Surgeon General Jerome Adams recently described the crisis the nation is facing as “our Pearl Harbor moment, our 9/11 moment.” Battling COVID-19, he said, has in many respects been like waging war.
Dr. Manni said the Surgeon General wasn’t mistaken.
“We’re fighting two things,” she explained. “We’re fighting the virus, but we’re also fighting to keep people calm and level-headed and focused on facts so that they’re not giving misinformation or acting on misinformation. And that’s tantamount to handling something like this.”
Dr. Zaidner said the pandemic has changed the way health care is being administered and that many of the measures being instituted to protect patients and providers will remain in place even after the virus subsides or a vaccine is developed.
“We’re all going to continue to be extra cautious washing our hands and wearing protective gear,” he said. “And I don’t doubt that in the future we’re all going to be wearing masks in our daily routines in the hospital. This will change our practice forever, but the change will be for the better.”



